A smoothie can do more than fill a glass. With the right ingredients, it can support fullness, steady energy, and the gut signals tied to appetite control. That is where resistant starch smoothies for GLP-1 come in.
Resistant starch is different from regular starch because it resists digestion in the small intestine. Instead, it reaches the colon, where microbes ferment it and help shape satiety signaling. In smoothie form, that makes it easy to use with cold ingredients, simple prep, and a texture that works well for daily routines.
This guide walks through the gut mechanics, the best ingredients, and a few practical recipes you can use right away.
The GLP-1 Pathway: How Gut Fermentation Signals Satiety
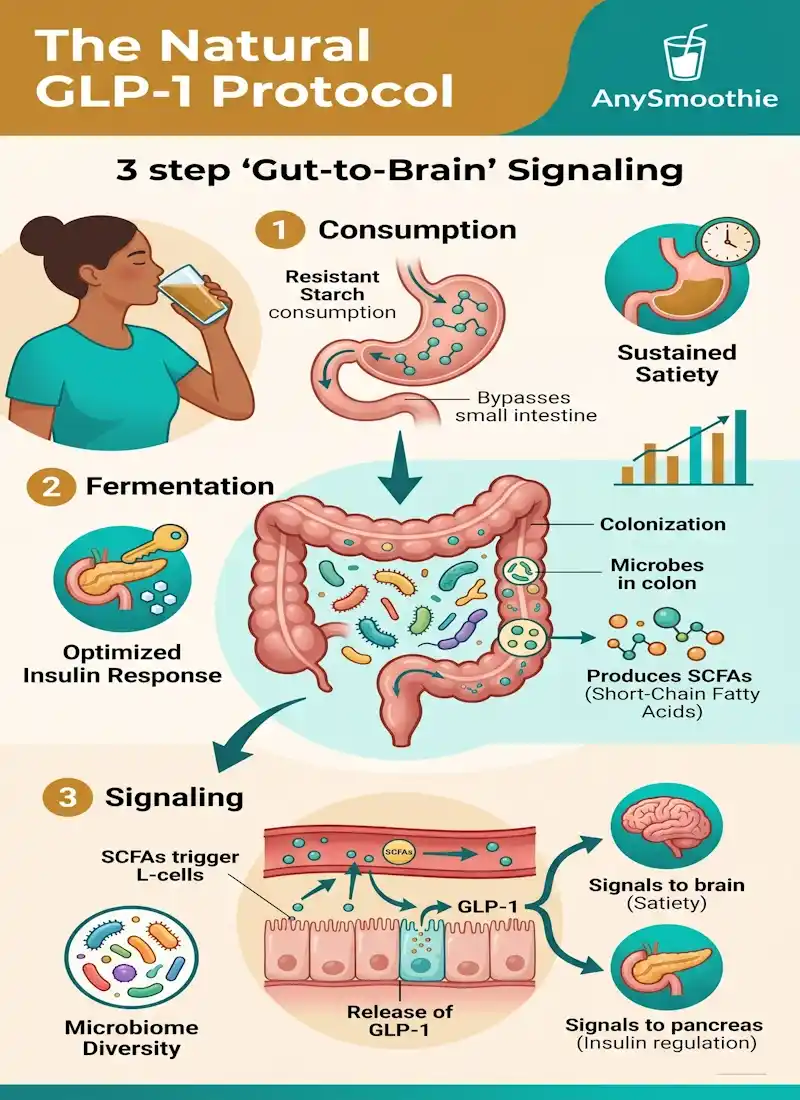
GLP-1 is part of the body’s appetite and glucose response system. It rises when the gut senses food, then sends signals that help manage how fast you eat, how full you feel, and how the next meal lands. Fiber and resistant starch matter because they do not disappear in the first stretch of digestion.
Instead, they move lower in the gut and meet the microbiome. There, bacteria ferment them and produce short-chain fatty acids, or SCFAs. That process is one reason resistant starch gets so much attention in metabolic health. A randomized trial in Scientific Reports linked resistant starch intake with changes in GLP-1-related responses and SCFA production, which fits this gut-first model of satiety support. You can see the study here.
These signals do not act alone. They work with stomach stretch, meal size, and the rest of your diet. Still, the fermentation step is the part that makes resistant starch different from a simple carb.
L-Cell Activation: The Role of Short-Chain Fatty Acids (SCFAs)
L-cells sit in the lining of the gut and respond to what reaches them. When SCFAs rise, those cells can support GLP-1 release and other satiety signals. Butyrate and propionate matter most here.
The effect is indirect, but important. Your smoothie feeds microbes first, then the microbes help shape the signal chain. That is why the same ingredient can feel different in a smoothie than in a sweet drink with fast sugar.
The best results come from ingredients that reach the lower gut, not just from a thick texture.
Resistant Starch Type 2: The Stealth Carbohydrate for Metabolic Flux
Resistant starch type 2, or RS2, fits smoothies well because it stays intact when it is used cold. Green banana flour is the most practical example. It has a mild taste, blends fast, and adds body without the sugar load of ripe fruit.
RS2 also behaves differently from fast starch. It passes through digestion with less immediate glucose impact, then gives the colon something useful to work with. That makes it a clean fit for people who want smoother energy and better meal spacing. It also pairs well with protein, fat, and spices, which help round out the flavor.
For smoothie use, the main job is simple: keep the starch raw, keep the drink cold, and keep the rest of the formula balanced. That is where texture meets function.
Propionate and Butyrate: The Biochemical Drivers of Incretin Release
Propionate and butyrate are the real workhorses here. They come from fermentation, and they help signal that the colon received useful fuel. Butyrate also supports the gut lining and local microbial balance.
That matters because GLP-1 support is strongest in the distal gut, where fermentation is active. The more your ingredients reach that zone, the more they can support natural incretin pathways. A review in Frontiers in Microbiology on resistant starch fermentation and butyrate production shows how much the response depends on the starch source and the gut environment. The paper is here.
Which GLP-1 Supporting Ingredients Work Best in Smoothies?
The right substrate depends on your goal. Resistant starch is strongest for distal-gut fermentation. Soluble fiber works more on bulk and slowing. Berberine-rich extracts act through a different metabolic route.
| Substrate | Physiological Mechanism | Primary Site of Action | Impact on Gastric Emptying | Best Smoothie Pairing |
|---|---|---|---|---|
| Resistant Starch (Green Banana Flour) | Butyrate signaling, SCFA production | Colon | Mild to moderate | Berries, kefir, cinnamon |
| Soluble Fiber (Psyllium/Inulin) | Water binding, microbiome support | Small intestine and colon | Moderate to strong | Yogurt, chia, cocoa |
| Berberine-rich Extracts | AMPK-related metabolic support | Systemic | Low to moderate | Unsweetened greens, citrus, protein |
The takeaway is simple. If you want a smoothie that works through fermentation, RS2 is the best fit. If you want more thickening and slower emptying, soluble fiber helps. If you want a different metabolic angle, berberine belongs in a separate plan, not as the main base.
3 ‘GLP-1 Prime’ Resistant Starch Smoothie Recipes
The “Satiety-Core” Green Banana Flour, Oat Bran, and Cinnamon Blend
This is the most balanced option for fullness and steady energy. Blend unsweetened almond milk, 1 to 2 tablespoons green banana flour, 2 tablespoons oat bran, cinnamon, ice, and a scoop of plain protein if you want more staying power.
Green banana flour brings RS2. Oat bran adds extra fiber and a softer texture. Cinnamon gives it warmth and helps keep the flavor grounded without added sugar. If you want a better taste, use vanilla extract and a few frozen berries. Keep the fruit modest so the drink stays lower in sugar.
A Berry and Kefir Version for a Lighter Gut-Friendly Option
Use kefir or another fermented base, a handful of berries, 1 tablespoon green banana flour, and a spoon of ground flax. This version is lighter and smoother, with a tangy taste that works well in the morning.
It also pairs resistant starch with fermented dairy or a probiotic base. Add a little nut butter or chia if you want more balance. That keeps the smoothie from feeling thin, which helps with satiety.
A Cacao and Almond Smoothie for Higher Satiety
For a richer drink, blend unsweetened almond milk, green banana flour, cacao powder, almond butter, ice, and a pinch of salt. This one feels more like a meal.
The fat from almond butter slows digestion. Cacao gives it depth without much sugar. Use this version when you want a denser texture and longer-lasting fullness.
Biohacking the Microbiome: Timing Starch Intake for Glucose Buffering
Timing changes how a smoothie behaves. In the morning, resistant starch can help set a steadier appetite pattern. Before lunch, it can take the edge off cravings. After a carb-heavy meal, it may help smooth the next glucose rise by shaping the response to the following meal.
That does not mean there is one perfect window. It means the timing should match your day. If breakfast is rushed, use it there. If lunch is your hardest meal, move it earlier. If evenings trigger snacking, test it before dinner instead.
Consistency matters more than chasing a precise minute on the clock.
Post-Prandial Precision: Reducing the Glycemic Response of Subsequent Meals
Post-prandial timing is simple. You eat, you digest, then you give the gut a fiber-rich or resistant-starch feed before the next meal. That can support a gentler glucose curve later on.
A practical pattern is to keep the smoothie small and use it as a buffer, not a sugar bomb. The goal is metabolic spacing, not constant grazing. Start with a small dose of resistant starch, watch how your gut feels, then adjust up slowly if you tolerate it well.
Conclusion
Resistant starch smoothies are a practical way to support gut signaling, satiety, and metabolic efficiency. They work best when you treat them as a tool, not a shortcut.
Start small, build tolerance, and choose ingredients that fit your goal, whether that is fullness, glucose support, or a calmer morning. If you want a simple place to begin, use green banana flour, a cold base, and one of the recipes above, then test the timing that fits your day.
⚠️ SAFETY NOTES: Resistant Starch for GLP-1
GASTROINTESTINAL ADAPTATION: Resistant starch is a potent prebiotic. Introducing 2 tablespoons at once can cause severe bloating, flatulence, and abdominal cramping as your microbiome shifts. Start with 1 teaspoon and increase the dosage over 2 weeks to allow for microbial adaptation.
TEMPERATURE SENSITIVITY: To maintain the RS2 structure (Type 2 Resistant Starch), do not heat your green banana flour or the smoothie. Heat causes “gelatinization,” converting the resistant starch into a rapidly digestible carbohydrate, which will spike your insulin instead of supporting GLP-1.
SIBO WARNING: If you have Small Intestinal Bacterial Overgrowth (SIBO), fermentable fibers like resistant starch can exacerbate symptoms (brain fog, extreme bloating, pain) by feeding bacteria in the wrong part of the digestive tract. Consult a specialist before use.
HYPOGLYCEMIA RISK: If you are taking GLP-1 agonist medications (like Ozempic or Wegovy) or insulin, adding a high-satiety, glucose-buffering smoothie can potentiate the effects, increasing the risk of hypoglycemia. Monitor your blood sugar closely.
KIDNEY HEALTH: Some green banana flours are high in potassium. If you have chronic kidney disease (CKD) and are on a potassium-restricted diet, check the nutritional label and consult your nephrologist.
FAQ
How does RS2 fermentation support the natural production of GLP-1?
Resistant Starch Type 2 (RS2) bypasses initial digestion in the small intestine to reach the distal colon, where it undergoes microbial fermentation. Biochemically, this process generates short-chain fatty acids (SCFAs), specifically butyrate and propionate, which act as signaling molecules. These SCFAs bind to receptors on enteroendocrine L-cells, supporting the physiological systems responsible for the natural release of GLP-1 (glucagon-like peptide-1), optimizing the body’s natural pathways of satiety and glucose regulation.
Why is the “Distal Gut” the primary site for incretin-related metabolic support?
The highest concentration of GLP-1 secreting L-cells is located in the distal ileum and colon. Supporting the physiological systems of this specific region requires nutrients like resistant starch that do not degrade in the upper GI tract. By ensuring that fermentable substrates reach the distal gut, you optimize the biochemical mechanics of incretin release, facilitating a more robust and sustained satiety signal compared to rapidly digestible carbohydrates.
How do Propionate and Butyrate act as biochemical drivers of satiety?
Propionate and butyrate are metabolic byproducts that serve as ligands for G-protein coupled receptors (such as fatty acid receptors) in the gut lining. This interaction supports the physiological systems involved in appetite suppression and insulin sensitivity. Biochemically, propionate can also influence hepatic glucose production, while butyrate provides fuel for colonocytes, ensuring that the natural pathways of metabolic flux and gut barrier integrity are maintained during nutrient partitioning.
What is the significance of “Mitochondrial Priming” in metabolic energy spacing?
Mitochondrial priming in a metabolic context refers to the cellular preparation required to efficiently oxidize fuel sources. Supporting the physiological systems of the gut-brain axis through resistant starch ensures that the influx of energy substrates is steady rather than erratic. This optimization prevents “metabolic congestion” in the mitochondria, ensuring that the natural pathways of ATP production are balanced and that the body can maintain efficient energy utilization between meals.
How does the “Second-Meal Effect” optimize post-prandial glucose responses?
The second-meal effect is a physiological phenomenon where the fermentation of resistant starch from a previous meal improves the glycemic response of the following meal. Biochemically, the production of SCFAs lowers the concentration of free fatty acids in the blood and supports the natural pathways of insulin sensitivity. By optimizing the gut environment in advance, you prime the physiological systems to handle subsequent glucose loads more efficiently, enhancing systemic metabolic resilience.

Medical Disclaimer: The information on AnySmoothie is for educational and informational purposes only. It is not intended as medical advice or a substitute for professional consultation with a healthcare provider. Always consult your physician before starting any new nutritional protocol, especially if you have underlying health conditions or are taking medication. By using this site, you agree to our full Disclaimer & Terms of Use.

